EMG & NCS: What do all these letters mean to the patient?
EMG & NCS: What do all these letters mean to the patient?
EMG & NCS. At first glance, the name of this study can easily confuse a patient. However, once it is broken down into its components, the words explain themselves. Electro-myo-graphy and Nerve Conduction Studies are, as the names state, electrical studies of the muscle “myo” and nerves. In a normal muscle, the electrical signal or waveform that is produced has a certain onset or latency, size or amplitude, duration, appearance, and sound. In muscles innervated by damaged nerves, the latency of the nerve may be delayed, amplitude may be abnormally large or small, and the clinician may hear certain sounds produced which indicate acute or chronic damage.
During the day-to-day routine in the clinical setting, we try to determine if a patient would benefit from an EMG/NCS through the process outlined below.
On our first evaluation of a patient, he or she may report numbness or tingling in one, two or all extremities with or without any pain complaints. At this point, the clinician should inquire about the duration of the patient’s symptoms, and exactly what areas are affected by the symptoms. Some of these questions may include:
- What time of day are symptoms present?
- Is the numbness and tingling worse at night or early mornings?
- Is the numbness and tingling related to certain activities?
- Are there any medications which alleviate the symptoms?
After obtaining the appropriate initial history, it is essential to review the patient’s medical history, as certain medical conditions can cause neuropathy affecting the sensory function of the nerves (which allow the patient to feel certain sensations). These medical conditions include diabetes, hypothyroidism, connective tissue disease, and alcohol consumption, among several others.
A thorough history is often followed by a physical examination of the patient, during which the clinician will focus on range of motion, muscle strength, muscle atrophy, and changes in sensation.
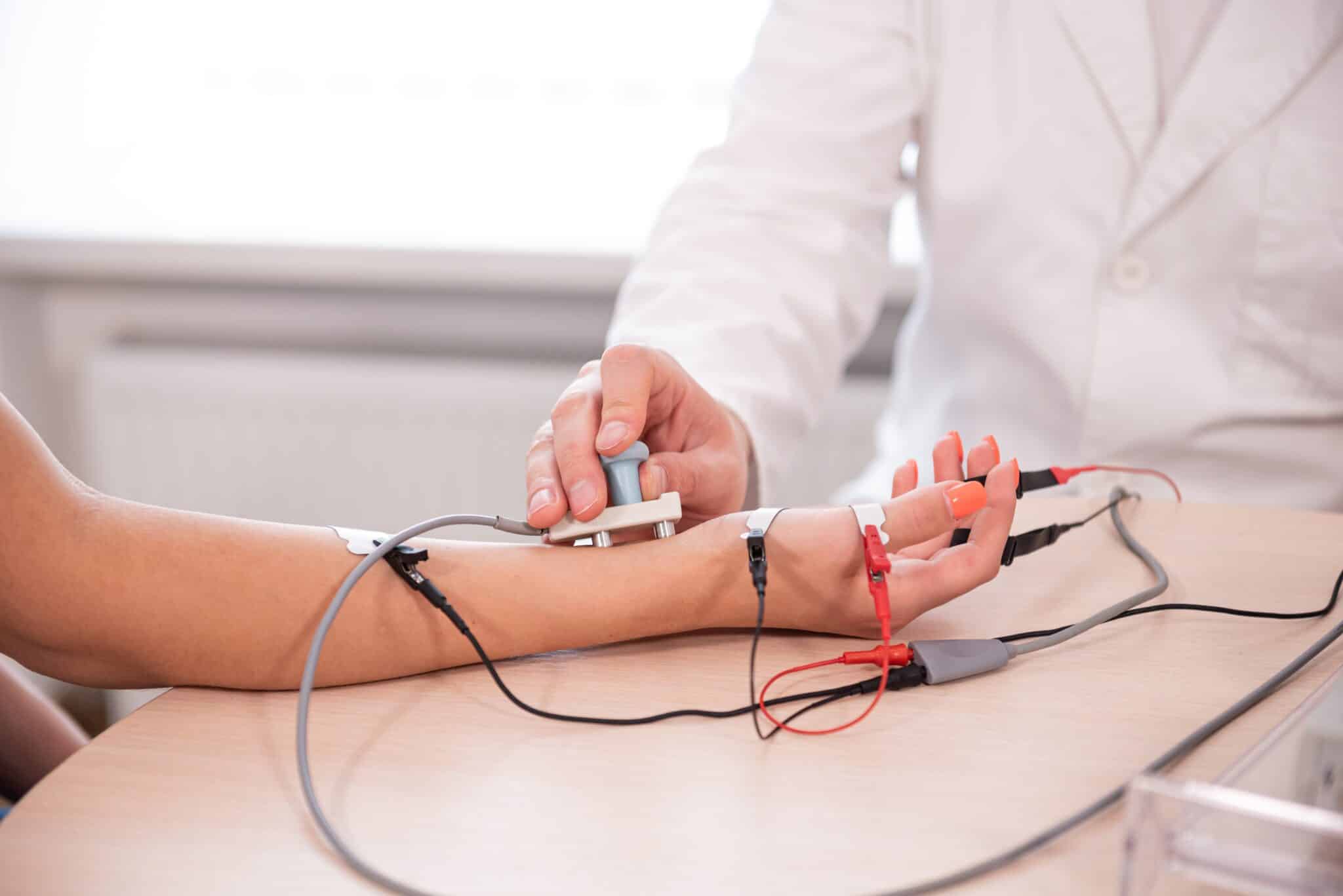
Once the determination is made that a patient has a clinical picture consistent with possible nerve damage, the EMG/NCS study is scheduled. The test generally starts with the NCS, or nerve conduction studies portion and involves the patient lying flat on a comfortable table. Then, grounding and recording wires, which are attached to gel-covered stickers, are placed directly on the skin. Therefore, it is essential that the patient does not apply any lotions or oils to the area to be tested. An electrical stimulator is applied to the skin, and then the patient feels a tingling sensation. Subsequently, a waveform is recorded from the particular nerve being tested, for the clinician to view and evaluate.
The second portion of the exam is the EMG, or electromyography, and focuses on testing the electrical activity of the muscle. A small, acupuncture sized needle is inserted into a particular muscle, and the clinician evaluates the size, shape, and sound of the signal. Based on the results of this evaluation, the clinician can diagnose a nerve problem in the arms, legs, or spine.
In summary, EMG & NCS is useful in the diagnosis of several conditions. Some of these include compressed nerves in the arms or legs (eg. Carpal Tunnel Syndrome or Tarsal Tunnel Syndrome), peripheral neuropathy (eg. Diabetic Neuropathy), and pinched nerves in the neck and back (radiculopathy). As with any diagnostic study, the findings of an EMG/NCS should be incorporated into the patient’s entire clinical picture.
Watch the video below to know what to expect during your EMG & NCS test.
Recent Posts
Turmeric for arthritis pain
December 10, 2025What is a Cervical Strain?
December 10, 2025How the Right Foods Help Ease Chronic Pain
November 26, 2024Share this Post