What is the cause of your back pain?
Low back pain, a ubiquitous condition that seems so familiar to everyone, has become ever so prevalent. It is common to hear of low back pain among parents, siblings, and even colleagues. Not surprisingly, neck and back pain is the leading musculoskeletal complaints that contribute to impairment and disability. Studies have shown that the lower back has a 5-10% annual incidence and 60-90% lifetime prevalence. In other words, there is a 5-10 % percent chance every year that a person may develop low back pain, and that percentage increases substantially to 60-90% chance of developing low back pain during his/her lifetime. Emergency rooms are notorious pit stops when patients develop such episodes of back pain. In fact, low back pain is one of the most common chief complaint documented during ER visits. It has been shown that approximately 50% of back pain tends to resolve in 1-2 weeks and 90% of low back pain tends to resolve in 6-12 weeks which accounts for acute low back pain.
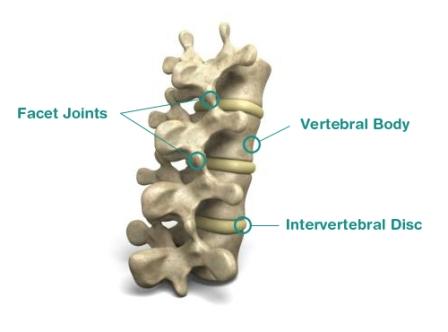
Generally speaking, if pain persists beyond 12 weeks it is considered chronic in nature. At this point, most acute ailments such as muscle spasm or back sprains tend to resolve. A deeper more introspective look may need to be done to examine the cause of such a persistent pain. A very basic overview of the spine classifies its weight bearing capacity into a 3 joint complex where weight is distributed on the intervertebral discs between the vertebral bodies and the posterior facet joints on the left and right side.
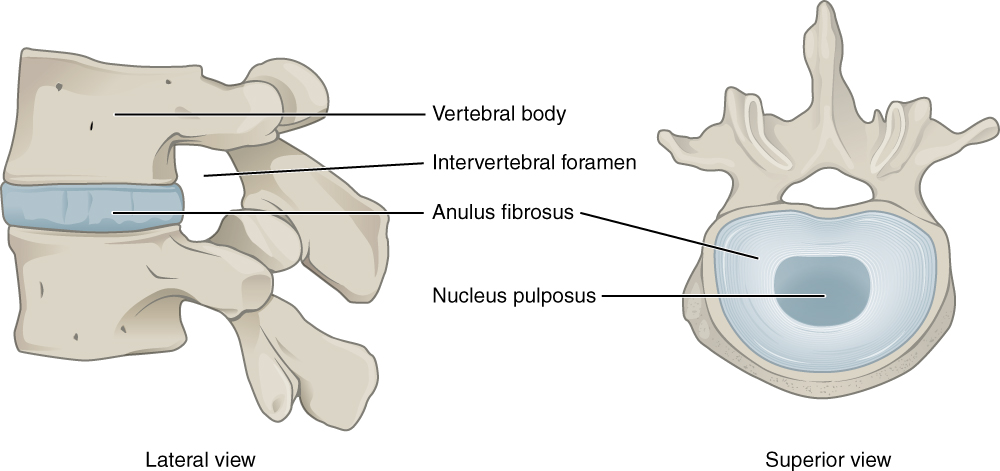
Intervertebral disks act as shock absorbers to the vertebral bodies and help provide height to the spine. The discs are made of an inner viscous jell material called the nucleus pulposus and outer annulus fibrosis made of connective tissue called collagen. Only the outer 1/3 of the annulus fibrosis contains nerve fibers, thus when discs deteriorate and the nucleus pulposus leaks into the annulus through a tear it is generally painful if it involves the outer 1/3 layer. Discs tend to become impacted with the loading of the spine and flexion based activities which place more stress on the disks.
Deterioration at the disks or degenerative disc disease can result in more stress placed on the posterior elements, otherwise known as the facet joints. Facet joints are posterior elements of the spine which help to provide further stability and movement of the spine. Similarly, like the disks, the facet joints on either side of the spinal segment play a central role in distributing the weight of the spine. Wear and tear of the facet joints can lead to arthritis just like other joints in the body and can result in associated paraspinal muscle spasms. Often patients will experience worsening pain in the cold weather due to the arthritic nature of the pain, and pain can be elicited with extension-based activities as well as lateral bending or rotation of the spine. The relationship of the disks and facet joints in the 3 joint complexes is not a mutually exclusive one as wear and tear of the facet joints, or facet arthropathy can impact the disks as well. These three joints are all susceptible to arthritis and can become potential causes for pain generators of the spine.
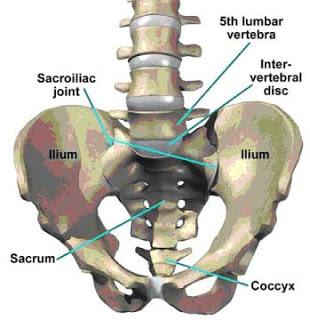
The sacral iliac joint is another joint seen at the articulation of the sacrum and ilium. The SI joint is also a weight-bearing joint that is located below the lumbar spine, and are located on the left and right side. Often those who have surgery or instrumentation in their lumbar spine are more susceptible to the pathology of the SI joints due to the alteration in the kinematics of the spine. With the removal of spinal bone and placement of hardware the normal weight-bearing areas of the spine have now shifted and the brunt of the impact is more steadily involved with the joints below, namely the SI joints. Provocative maneuvers may help elicit SI joint pain as a diagnosis, but generally speaking, an intraarticular joint injection is the gold standard in diagnosing it as pain should immediately improve if it is the primary generator of pain.
The pain generators of the spine include discogenic pain, facet mediated joint pain, sacral-iliac joint pain, and vertebral pain. Taking age into account may help to better delineate the causes of these pain generators. Generally intractable back pain in the elderly tends to be more consistent with arthritis which is most pronounced in the posterior facet joints. Whereas younger patients tend to have discogenic back pain due to strenuous activities involving the loading of the spine. The median age of onset for various pain generators have been documented with facet joint pain at 59, disc related pain 36.7, and sacral iliac joint pain at 32.8 The overall prevalence of these generators have been documented with discogenic pain at approximately 48%, facet joint pain of 31%, SI joint pain 18.2% and vertebral pain of 2.9%.
As one can see there is a lot more than meets the eye when evaluating chronic back pain. This is just a basic overview that should give you more insight into the causes and implications of back pain.
Recent Posts
How the Right Foods Help Ease Chronic Pain
November 26, 2024Workplace Pain Relief and Management: The Best Ways to Diminish Pain
February 12, 2020Knee Pain — Healing for Health and Happiness, Capitol Pain
December 12, 2019Share this Post
